What if I told you that there is a decision you can make for your unborn baby that has the potential to drastically increase his quality of life for years to come that is FREE and takes only 90 seconds to implement? Unbelievable, right?
Dr. Alan Greene does an amazing job explaining the important concept I want to introduce to you today in this 15 minute TED talk. I encourage you to watch it first if you can (it’s really well done), but if you are in a hurry, just skip down a bit for a recap and more details.
Good Intentions Aren’t Enough
In 1913 an idea took hold in the medical community that has potentially decreased the intelligence, productivity, and “quality adjusted life years” of people worldwide. To prevent postpartum hemorrhage and facilitate treatment or resuscitation of babies in distress, it was decided that the “third stage of labor” (birth of the placenta) needed to be actively managed by:
- routine use of drugs like pitocin to stimulate contractions and release the placenta
- immediate cord clamping (and separation of baby and mother)
- controlled cord traction (pulling the placenta out)
These measures have become common practice among care providers. Despite good intentions, each one has negative unintended consequences to weigh. Immediate cord clamping in particular poses risks that have been under-emphasized and need to be brought to light.
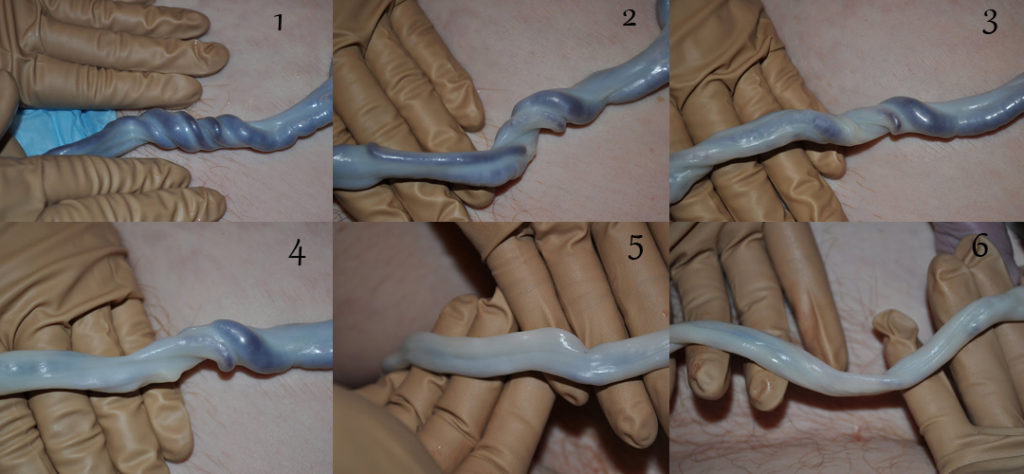
When a baby is born, one third of his blood volume is outside his body! While in utero, the umbilical cord routes all of the nutrients and oxygen baby needs from mother – through the placenta. Generally, the placenta is still attached when the baby is born, and for a time – 3-5 minutes or longer – the placenta and cord continue to pump blood back into the baby.
The photo collage above is a great example of this process – these photos were taken over a 15 minute period. (you can read more from the source here) Waiting to clamp and cut the umbilical cord means your baby receives 1/3 more life-giving blood!
More Cord Blood Means:
More Oxygen
The blood flowing through the umbilical cord is rich in oxygen and babies’ brains continue to benefit from it even after their lungs have filled the first time. As Dr. Greene points out in the video,1 out of 10 children in the world get sub-optimal amounts of oxygen in the first few minutes of life. This leads to problems ranging from decreased intelligence to cerebral palsy.
More Iron
The WHO claims that about 25% of the world’s population suffers from anaemia – many due to iron deficiency. Immediate cord clamping increases the risk of developing Iron Deficiency Anaemia by 10 times! Iron deficiency is also the most common nutritional deficiency in the world, and preventing it would increase national productivity 20%.
More White Blood Cells
Increasing the baby’s blood volume means more disease-fighting white blood cells. Neonatal Sepsis (infection in a newborn) is a major killer – especially in low-resource communities. More blood means a stronger defense (without any added cost).
More Stem Cells
You can’t pick up a pregnancy magazine without seeing two or three full page ads for stem cell banks these days. We don’t yet know exactly how important stem cells are or how they will be used, but the potential is great. For an insightful look at the pros and cons of banking your baby’s cord blood as well as a couple of wonderful videos, I recommend this post by Midwife Thinking. If you choose not to use a cord blood bank, you can still gift your baby with more stem cells by waiting to clamp his cord.
“Delayed” Cord Clamping?
In his TEDx talk, Dr. Greene introduced his initiative called TICC TOCC – which stands for Transitioning Immediate Cord Clamping To Optimal Cord Clamping. He asks care providers to wait as little 90 seconds, or until the cord stops pulsing, before clamping. The current standard of 25 or so seconds is what he calls “immediate,” but he hesitates to use the term “delayed cord clamping,” opting instead for “optimal cord clamping.”
“Not only have people around the world traditionally waited for the cord to stop pulsing until the 20th century innovation, every other mammal studied instinctively waits for the cord to stop pulsing as well.” Dr. Alan Greene
With birth plans becoming more common and the ability to easily spread information via the internet, hopefully care providers will soon become more aware of the benefits of Optimal Cord Clamping. If you know someone who may not have read about OCC, please consider directing them to this post or to Dr. Greene’s TICC TOCC campaign.
How long did you wait before clamping the umbilical cord?
More Resources:
5 Simple Tips for Writing a Birth Plan
WHO optimal timing recommendation
Common Objections to Delayed Cord Clamping – Science & Sensibility





Okay, I am all for delayed cord clamping. I even had it in my birthplan. However, when my baby was born the nurse started to clamp the cord, I told her to wait, and she did it anyway. So what do I do now? Obviously I can’t undo the early cord clamping, but is there anything I can do to negate the negative side effects of early cord clamping?
We did this with our fourth child (would have sooner if I’d heard about this). He became quite jaundiced later and the doctor said he needed to go under that bilirubin light for two days. To avoid this with the next baby, any ideas? Doctors can be good at “guilting” you into those lights. From what I read at the time (4 years ago), waiting to clamp can cause those bilirubin levels to climb. I’m all for it and will wait till the cord stops pulsing with our next baby but need to know more of what to do with the whole bilirubin-thing if that comes up again. Baby will be born in January so no real sunlight available where we live. All our babies have nursed on demand (ie. a lot! lol). Thanks for the great post!
We chose to delay the cord clamping with both our boys. Both had mild jaundice, which I determined was a benign result of the increase in red blood cells, but worth it. We’ve learned to check bilirubin on day 4, when it typically peaks (not the hospital’s immediate or next-day routine), to be sure levels have dropped to normal range. I also enjoyed a few sun walks with my newborns as soon as possible. 😉
Our midwife with Greyson was able to collect blood for banking even after the cord stopped pulsating (>2 min), but with Benjamin the nurse and doctor completely botched the banking. They didn’t seem comfortable delaying the clamping AND banking the blood, even after claiming they could do it. I highly recommend parents be sure the professionals involved have had experience with either one or both of these procedures (delayed clamping and banking). Cord blood can be successfully banked after delayed or “optimal” clamping, with a supportive and experienced OB or midwife.
My OB was supportive of optimal clamping, but I ended up with an emergency C-section. The doctor told me later they can’t wait to clamp/cut the cord in that situation because their priority is stopping my bleeding, but my husband seems to think they could have at least cut the cord closer to the placenta end and let gravity push the extra blood into the baby. Any thoughts on what to do if I end up in this situation again with Baby #2?
I will be having a C-section in November. Not my first choice, but medically necessary for me and baby this time 🙁 My doctor said they don’t do delayed cord clamping during C-sections, but they do ” milk ” the cord to get the blood to go into baby before they clamp. Any ideas on this?
Thank you, the article does answer some questions.
[…] 90 Seconds That Could Change Your Baby’s Life […]
[…] 90 Seconds Could Change Your Baby’s Life […]
[…] Thoughts on Circumcision: AKA Why I’m Glad I’m Having a GirlNewborn Procedures: Hepatitis B90 Seconds That Could Change Your Baby’s Life […]
[…] in its own time with the help of the mother
[…] When I had my first child, the plan was to delay the clamping of the cord until it stopped pulsating. We had planned on being at home for his birth, but due to circumstances we ended up at the hospital. After the placenta was delivered the nurse immediately clamped the cord. My son, who was premature and ended up needing to be in the NICU for eight days, lost out on the benefits of delayed cord clamping. Learn more about the benefits of delayed cord clamping here. […]
This is a very useful article. Its amazing how a few extra minutes can make such a huge difference for the baby. Thanks for this article. Also I came across http://www.whattoexpect.com/pregnancy/fetal-development/fetal-brain-nervous-system/ while researching and found it really helpful. Hope this helps your readers too.